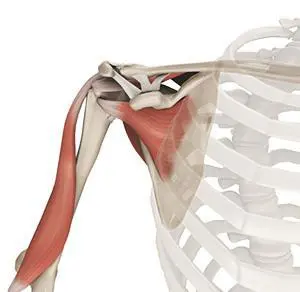
Shoulder
SHOULDER ANATOMY
The shoulder is the most flexible joint in the body that enables a wide range of movements including forward flexion, abduction, adduction, external rotation, internal rotation, and 360-degree circumduction. Thus, the shoulder joint is considered the most insecure joint of the body, but the support of ligaments, muscles, and tendons function to provide the required stability.
Bones of the Shoulder
The shoulder joint is a ball and socket joint made up of three bones, namely the humerus, scapula, and clavicle.
Humerus
The end of the humerus or upper arm bone forms the ball of the shoulder joint. An irregular shallow cavity in the scapula called the glenoid cavity forms the socket for the head of the humerus to fit in. The two bones together form the glenohumeral joint, which is the main joint of the shoulder.

Scapula and Clavicle
The scapula is a flat triangular-shaped bone that forms the shoulder blade. It serves as the site of attachment for most of the muscles that provide movement and stability to the joint. The scapula has four bony processes – acromion, spine, coracoid and glenoid cavity. The acromion and coracoid process serve as places for attachment of the ligaments and tendons.
The clavicle bone or collarbone is an S-shaped bone that connects the scapula to the sternum or breastbone. It forms two joints: the acromioclavicular joint, where it articulates with the acromion process of the scapula and the sternoclavicular joint where it articulates with the sternum or breast bone. The clavicle also forms a protective covering for important nerves and blood vessels that pass under it from the spine to the arms.
Soft Tissues of the Shoulder
The ends of all articulating bones are covered by smooth tissue called articular cartilage, which allows the bones to slide over each other without friction, enabling smooth movement. Articular cartilage reduces pressure and acts as a shock absorber during movement of the shoulder bones. Extra stability to the glenohumeral joint is provided by the glenoid labrum, a ring of fibrous cartilage that surrounds the glenoid cavity. The glenoid labrum increases the depth and surface area of the glenoid cavity to provide a more secure fit for the half-spherical head of the humerus.
Ligaments of the Shoulder
Ligaments are thick strands of fibers that connect one bone to another. The ligaments of the shoulder joint include:
- Coracoclavicular ligaments: These ligaments connect the collarbone to the shoulder blade at the coracoid process.
- Acromioclavicular ligament: This connects the collarbone to the shoulder blade at the acromion process.
- Coracoacromial ligament: It connects the acromion process to the coracoid process.
- Glenohumeral ligaments: A group of 3 ligaments that form a capsule around the shoulder joint and connect the head of the arm bone to the glenoid cavity of the shoulder blade. The capsule forms a watertight sac around the joint. Glenohumeral ligaments play a very important role in providing stability to the otherwise unstable shoulder joint by preventing dislocation.
Muscles of the Shoulder
The rotator cuff is the main group of muscles in the shoulder joint and is comprised of 4 muscles. The rotator cuff forms a sleeve around the humeral head and glenoid cavity, providing additional stability to the shoulder joint while enabling a wide range of mobility. The deltoid muscle forms the outer layer of the rotator cuff and is the largest and strongest muscle of the shoulder joint.
Tendons of the Shoulder
Tendons are strong tissues that join muscle to bone allowing the muscle to control the movement of the bone or joint. Two important groups of tendons in the shoulder joint are the biceps tendons and rotator cuff tendons.
Bicep tendons are the two tendons that join the bicep muscle of the upper arm to the shoulder. They are referred to as the long head and short head of the bicep.
Rotator cuff tendons are a group of four tendons that join the head of the humerus to the deeper muscles of the rotator cuff. These tendons provide more stability and mobility to the shoulder joint.
Nerves of the Shoulder
Nerves carry messages from the brain to muscles to direct movement (motor nerves) and send information about different sensations such as touch, temperature, and pain from the muscles back to the brain (sensory nerves). The nerves of the arm pass through the shoulder joint from the neck. These nerves form a bundle at the region of the shoulder called the brachial plexus. The main nerves of the brachial plexus are the musculocutaneous, axillary, radial, ulnar and median nerves.
Blood vessels of the Shoulder
Blood vessels travel along with the nerves to supply blood to the arms. Oxygenated blood is supplied to the shoulder region by the subclavian artery that runs below the collarbone. As it enters the region of the armpit, it is called the axillary artery and further down the arm, it is called the brachial artery.
The main veins carrying de-oxygenated blood back to the heart for purification include:
- Axillary vein: This vein drains into the subclavian vein.
- Cephalic vein: This vein is found in the upper arm and branches at the elbow into the forearm region. It drains into the axillary vein.
- Basilic vein: This vein runs opposite the cephalic vein, near the triceps muscle. It drains into the axillary vein.
ORTHOBIOLOGICS FOR SHOULDER PAIN
The Healthy Shoulder
The shoulder is a ball and socket joint made up of three bones, namely the humerus, scapula, and clavicle. The ends of all articulating bones are covered by smooth tissue called articular cartilage which allows the bones to slide over each other without friction enabling smooth movement.
The ligaments of the shoulder joint include coraco-clavicular ligaments, acromio-clavicular ligament, coraco-acromial ligament, and glenohumeral ligaments. The rotator cuff is the main group of muscles in the shoulder joint and is comprised of 4 muscles. The deltoid muscle forms the outer layer of the rotator cuff and is the largest and strongest muscle of the shoulder joint. Two important groups of tendons in the shoulder joint are the biceps tendons and rotator cuff tendons.
Shoulder Injuries
The shoulder is the most flexible joint in the body enabling a wide range of movements. The most common shoulder injuries/diseases include
- Shoulder Arthritis
- Rotator Cuff Injury
- Shoulder Bursitis
- Glenoid Labrum Tear
- Inflamed Synovial Membrane
Orthobiologics
Progenitor cells are present in all of us acting like a repair system for the body. However, with increased age sometimes the optimum amounts of these cells are not delivered to the injured area. The goal of orthobiologic treatment is to amplify the natural repair system of the patient’s body.
Preparing for the Procedure
It is important that you stop taking any non-steroidal anti-inflammatory drugs (NSAIDs) at least two weeks before your procedure.
Preparing for a orthobiologic procedure is relatively easy and your doctor will give you specific instructions depending on your condition.
Orthobiologic Procedure
The procedure begins with your doctor extracting progenitor cells, and growth factors from either your blood (PRP/PRF), bone marrow, or adipose tissue (fat). After the tissue is harvested it is cleaned and then separated using sterile processing. It is then ready to be used to heal your injured joint or soft tissues.
Your doctor then cleans and numbs your affected area to be treated and then, under the guidance of special x-rays, injects the concentrate into the diseased region. The whole procedure usually takes less than one hour and you may return home on the same day of the procedure.
Post-Operative Care
- You will most likely be able to return to work the next day following your procedure.
- You will need to take it easy and avoid any load bearing activities for at least two weeks following your procedure.
- You will need to refrain from taking non-steroidal, anti-inflammatory medications (NSAIDS) for a while as this can affect the healing process of your body.
Risks and Complications
This procedure is generally considered a safe procedure with minimal complications, however, as with any medical procedure, complications can occur.
Some of the complications related to ortho biologic therapy include pain at the donor site which usually resolves in 2 to 3 days, swelling at the injection site, bruising at the donor site, bleeding and stiffness. There is a very small risk of infection following these injections which in my experience is much less than 1%.